Pancreas And Multi Visceral Transplantation
What is a pancreas transplant?
Although often performed as a last resort, the pancreas transplant has become a key treatment for people with type 1 diabetes. Pancreas transplants are also sometimes carried out in people who require insulin therapy and have type 2 diabetes. However, this is much less common.
The first human pancreas transplant was completed in 1966. The United Network for Organ Sharing (UNOS) reports that have been performed in the United States between January 1988 and April 2018.
The aim of a transplant is to restore normal levels to the body. The transplanted pancreas is able to produce insulin to manage blood glucose levels. This is a task that a transplant candidate’s existing pancreas can no longer perform properly.
A pancreas transplant is mainly done for people with diabetes. It typically won’t be used to treat people with other conditions. It’s rarely done to treat certain cancers.
Who donates the pancreas?
A pancreas donor is usually someone who’s declared brain-dead but remains on a life-support machine. This donor has to meet common transplant criteria, including being a certain age and otherwise healthy.
The donor’s pancreas also has to match immunologically with the recipient’s body. This is important to help reduce rejection risk. Rejection occurs when a recipient’s immune system reacts adversely to the donated organ.
Occasionally, pancreatic donors are living. This may happen, for example, if the transplant recipient can find a donor who’s a close relative, such as an identical twin. A living donor gives part of their pancreas, not the whole organ.
What happens before a pancreas transplant?
You’ll receive a medical evaluation at a transplant center before any sort of organ transplant. This will involve multiple tests to determine your overall health, including a physical exam. A healthcare professional at the transplant center will also review your medical history.
Before you receive a pancreas transplant, specific tests you may undergo include:
* blood tests, such as blood typing
* achest X-ray
* kidney function tests
* neuropsychological exams
* studies to check your heart function, such as an echocardiogram or electrocardiogram (EKG)
This evaluation process will take one to two months. The goal is to determine whether you’re a good candidate for surgery and whether you’ll be able to handle the post-transplant drug regimen.
If it’s determined that a transplant will be appropriate for you, then you’ll be placed on the transplant center’s waiting list.
Keep in mind different transplant centers will likely have different preoperative protocols. These will also vary further depending on the type of donor and overall health of the recipient.
How is a pancreas transplant performed?
If the donor is deceased, your surgeon will remove their pancreas and an attached section of their small intestine. If the donor is living, your surgeon will usually take a portion of the body and tail of their pancreas.
A PTA procedure takes around two to four hours. This procedure is carried out under general anesthesia, so the transplant recipient is fully unconscious throughout to not feel any pain.
Your surgeon makes a cut down the center of your abdomen and places the donor tissue in your lower abdomen. They’ll then attach the new section of the donor small intestine containing the pancreas (from a deceased donor) to your small intestine or the donor pancreas (from a living donor) to your urinary bladder and attach the pancreas to blood vessels. The recipient’s existing pancreas usually remains in the body.
Surgery takes longer if a kidney is also transplanted via an SPK procedure. Your surgeon will attach the donor kidney’s ureter to the bladder and blood vessels. If possible, they’ll usually leave the existing kidney in place.
What happens after a pancreas transplant is performed?
Post-transplant, recipients stay in the intensive care unit (ICU) for the first few days to allow close monitoring for any complications. After this, they often move to a transplant recovery unit within the hospital for further recuperation.
A pancreas transplant involves many types of medications. A recipient’s drug therapy will require extensive monitoring, especially since they’ll take a number of these drugs every day to prevent rejection.
What is a Multi Visceral Transplantation?
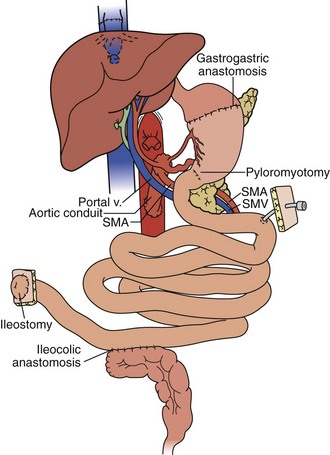
The transplantation of multiple abdominal viscera, including liver-duodenum-pancreas, liver-stomach-duodenum-pancreas and liver-intestine, is being performed with increasing frequency and success. These procedures and other variations are derived from a seldom used multivisceral operation in which all of the foregoing organs are transplanted en bloc.
It is described herein how the full multivisceral transplantation and its less extensive derivatives are based on the same principles of procurement, preservation and postoperative management. With all of these multiple organ permutations and with intestinal transplantation alone, management is complicated by inclusion in the grafts of a large lymphoreticular component that is capable of causing graft versus host disease (GVHD). Because of a systematic error in therapeutic philosophy, past efforts have been directed at altering or damaging the lymphoreticular cells by pretreatment of the donor or of the organs with drugs, irradiation or other means.
From recent observations, the alternative approach is suggested of keeping these lymphoid depots intact, which then become the site of two way cell traffic after transplantation. With the use of powerful immunosuppression, such as that provided with FK 506, the donor lymphoreticular cells can circulate in the recipient without causing clinical GVHD, and the lymphoreticular cells in the graft become those of the recipient (local chimerism) without causing rejection. Even with avoidance of rejection and GVHD, metabolic interrelations between the grafted organs, and also between the graft organs and retained recipient viscera can affect the fate of the individual transplanted organs or retained recipient organs.
The best delineated of these metabolic influences are mediated by the endogenous splanchnic hepatotrophic factors, of which insulin has been the most completely studied. An understanding of these various immunologic and nonimmunologic factors combined with more potent immunosuppression that is now available is sure to stimulate efforts at transplantation of abdominal organs and particularly of the hollow viscera that have resisted such clinical efforts.
Multivisceral transplantation having more than three abdominal organs replacement such as stomach, duodenum, pancreas, small intestine, and liver. The transplantation is based on patients need.
The pancreas lies behind the lower part of the stomach. The main function of the pancreas is to create insulin. Insulin is a hormone responsible to regulate sugar (glucose) absorption into the body. If the pancreas is unable to create enough insulin, then sugar level increases to an unnatural level resulting in diabetes. A pancreas transplant is used to overcome this condition.
Pancreas transplantation is for people who suffer from chronic diabetes and also have renal failure. It is aimed to ‘cure’ diabetes and in the long run, it will protect the transplanted kidney from being affected by diabetes and even reverse neuropathy and prolong their life. Dr. Bipin Vibhute is the best for Pancreas Transplant in Pune, Maharashtra.
Small bowel transplantation is for people with bowel failure from either surgical cause or medical cause. Bowel failure means bowel is unable to absorb nutrients from food. Sometimes people need their nutrition to be fed through a drip into a vein as their bowel is unable to absorb nutrients from any food. This patient population, if not treated appropriately treated will develop liver and or kidney failure.
They will need a combination of liver, small intestine and kidney transplantation (multi-visceral transplantation). We have a successful on-going cadaver organ transplantation program which will make these types of complex operations possible. Moreover, we have the doctors and the technology available to optimize their care in all the aspects.
